Another One Added to Wrong Patient Surgery Cases – Is Patient Misidentification To Blame?
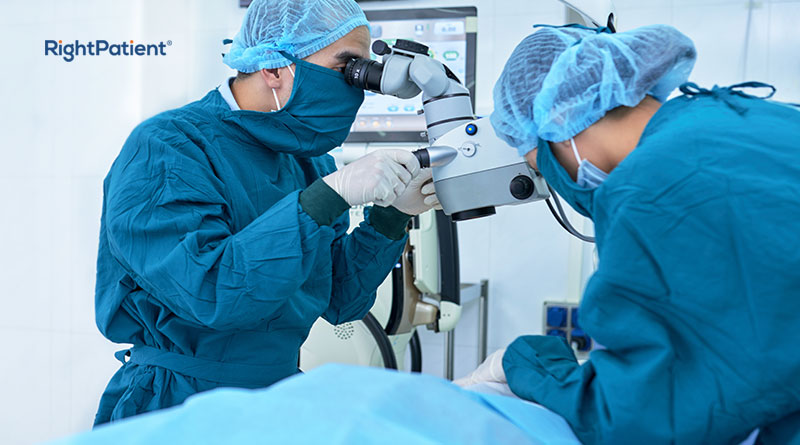
We’ve been talking about patient misidentification for quite a long time now, and for very good reasons. While many think that patient identification errors in hospitals are not that common or serious, but every now and then, a piece of news comes up that shows just how serious it can be. This time, a patient received a kidney that was actually meant for someone else – can you imagine? Without further ado, let’s dive deep into the unfortunate tale and see how wrong patient surgery cases can be prevented with positive patient identification.
A classic case of transplant mix-up
This unfortunate case of transplant mix-up is exactly what we warn healthcare professionals against – we’ve seen our fair share of wrong patient surgery cases.
It occurred in University Hospitals (UH) on the 2nd of July, and fortunately, the recipient survived, as the kidney was compatible with the patient. The patient is slowly recovering, according to a spokesperson, and the surgery of the actual patient who was supposed to get the kidney has been delayed. UH also notified UNOS (United Network for organ Sharing) about the transplant mix-up.
Moreover, UH isn’t divulging any more details about the situation as of now – they are analyzing the situation, investigating what caused the issue, and are working so that it never occurs again. However, the employees that were involved with the medical error are on administrative leave until the issue is figured out.
However, while this might seem quite unusual, wrong patient surgery cases do occur every now and then – something which we can confidently say occurs because of patient mix-ups due to poor patient identification systems.
Wrong patient surgery cases are uncommon, but not unheard of
Back in 2019, before the pandemic changed everything, wrong patient identification led to another transplant mix-up in Lourdes Hospital Transplant Center (which we’ve covered already). Coincidentally, it also was a case of a kidney transplant.
However, this was a much more transparent case as the patients had a similar name and age – something that we very well know leads to patient mix-ups, among other things. Fortunately, in that case, the patient who got the kidney survived as it was a perfect match.
This case was also reported to UNOS and the patient who was supposed to get the kidney had the transplant down the line.
However, in UH’s case, the patient who’s supposed to get the transplant is still on the waiting list. As already mentioned, UH isn’t releasing any details about the mix-up – but we are too familiar with such cases.
Wrong patient surgery cases occur due to poor patient identification
In Lourdes Hospital Transplant Center’s case, the patients had common names and were of similar age. This is a classic case of patient identification errors. Patient’s medical records are usually mixed up during registration, and if they have common characteristics, such devastating cases are generated.
We believe that whatever occurred in UH was due to patient misidentification, or the lack of proper patient identification.
Medical record mix-ups, poor quality patient data, medication administration errors, wrong transplants, detrimental healthcare outcomes, mistreatments, and adverse incidents are just some of the consequences of poor patient identification, and can even claim patients’ lives. The patients involved in the two wrong patient surgery cases above are extremely lucky to be alive – not everyone makes it out alive.
Such transplant mix-ups or patient mix-ups are deadly, but they ARE preventable – as long as the healthcare provider is ensuring accurate patient identification. We’re so concerned about such cases is because we help responsible hospitals and health systems prevent patient mix-ups with our industry-leading touchless biometric patient identification platform, RightPatient.
RightPatient prevents patient mix-ups and patient safety incidents
RightPatient prevents patient identification errors right from the start. It takes patients’ photos during registration and locks the medical records with them. Whenever a patient comes up later on, the platform provides the accurate medical record after comparing the saved photo with the live one. This makes sure that patient mix-ups are eliminated, as it uses the one characteristic that cannot be mixed up – patients’ faces.
RightPatient has a vast amount of experience with ensuring accurate patient identification in several hospitals and health systems, and we’re confident that it could’ve prevented such cases.
Are you preventing such mix-ups at your healthcare facility effectively?

























 RightPatient is the healthcare industry’s leading photo-based biometric
RightPatient is the healthcare industry’s leading photo-based biometric

