Tips for Maintaining Patient Health and Well-Being with Tech

Technological advances are creating seismic changes in virtually every industry, and healthcare is no exception. Providing effective patient care can present a number of significant challenges that have historically plagued the healthcare system at large.
These issues have incurred severe costs over time in the form of wasted resources, care failures, and even lives in many cases.

Applying technology to solving these problems can fundamentally change the quality and effectiveness of the healthcare system. One area of healthcare that is experiencing particular innovation is that of patient health and well-being. Thanks to technological trends and advances over the past five years, our capabilities in this area have skyrocketed.
In this article, we’ll explore the top areas where tech is revolutionizing patient care.
Why Maintaining Patient Health and Well-Being is Vital
It could be argued that maintaining patient health and well-being is the single fundamental purpose of the healthcare system at large. However, there are several practical and operational ways of understanding this concept that help distinguish patient health and well-being from other systems within healthcare. Maintaining effective protocols for ensuring patient health and well-being is important in a few ways.
Patient health and well-being directly contribute not only to patient outcomes (e.g. the ultimate effectiveness of the treatment or care they receive) but to the patient’s experience and perception of the care they receive. Ultimately, not only the individual patients but healthcare providers, friends and family, and other stakeholders all benefit from favorable patient experiences.
Mitigating lawsuits, decreasing workplace stress for medical professionals, and increasing long-term engagement with healthcare are just some of the advantages the healthcare system can experience when it prioritizes patient health and well-being during the care process.
Top Technological Solutions Raising the Bar for Patient Health and Well-Being
Technology can be used to increase the average level of patient health and well-being in several ways. Here are a few of the top strategies for approaching this goal (though this is not an exhaustive list):
Leveraging the Power of Electronic Health Records (EHRs) and Patient Identification Tools
Having systems in place to better maintain and access patient records while providing care can create a number of benefits for both patients and medical professionals. Having a patient’s health history and profile information immediately available while providing care can help medical personnel avoid making costly mistakes or misdiagnoses.
A touchless patient identification platform like RightPatient helps prevent patient safety issues, misdiagnoses, and duplicate medical records. RightPatient utilizes biometrics to identify patient records accurately each time patients come in for visits (both physical and telehealth), preventing mix-ups, duplicate EHRs, and more.
It can also save time by mitigating redundant tests or procedures. This can improve patient outcomes and can also improve their experiences while receiving care.
Implementing Biotech Tools for Better Monitoring and Data Capture
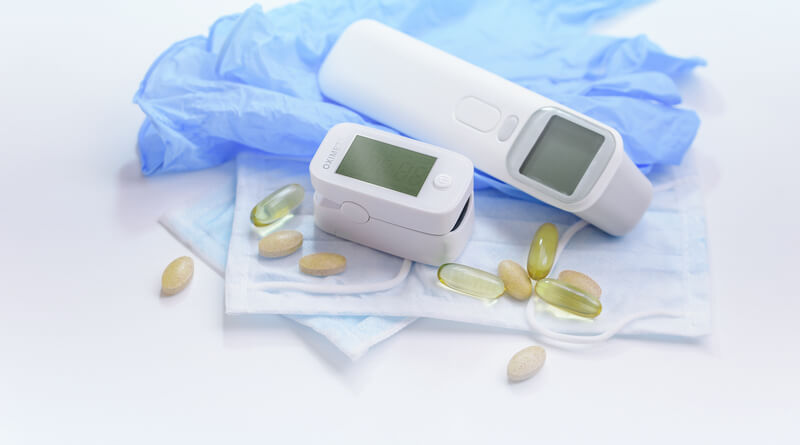
The prevalence, quality, and availability of consumer-accessible biotech and medical monitoring tools have reached unprecedented levels. This makes self-monitoring and new approaches to instituting care possible that utilize more sustained, accurate, or multifaceted data.
Tools for tracking blood pressure, heart rate, stress levels, sleep quality, blood samples, and more can be used by patients at home and in their daily lives. The resulting insights can much improve diagnosis as well as the treatment plan development process.
Utilizing Highly Viable Telehealth Options
Telehealth capabilities have also experienced rapid improvements and scaling over the past 3-5 years. This was partly propelled by necessity during the COVID-19 pandemic. The quality of telehealth services has made telehealth care an accessible, understandable, and preferred option for many patients across the country.
While telehealth won’t completely replace in-person healthcare provision (at least for the foreseeable future), it provides a helpful option for many patients and healthcare entities that can make certain types of healthcare provision much more efficient and convenient for both patients and care professionals.
Telehealth will likely be implemented in increasing measures, both to complement and replace certain types of in-person care, as the healthcare system continues to evolve.
Increasing Medical Professionals’ Access to Databases and Resources
The internet and its organization of information into accessible, centralized places have changed the way medical professionals can access medical knowledge. This can change the process of healthcare provision as well as increase its quality.
Doctors can use a medical prescription database on their phones to check instantly for drug incompatibilities or allergy dangers when writing prescriptions. Nurses can pull up the latest research from a medical database to answer a patient’s questions on the spot. Medical journals can be instantly cross-referenced to provide helpful insights when diagnosing a difficult case.
The wealth and accessibility of medical information and data have fundamentally changed the game for the healthcare process.
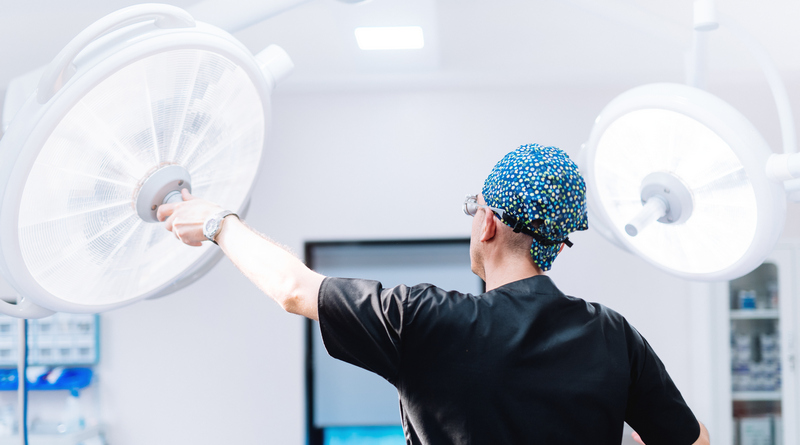
Integrating Artificial Intelligence (AI) and Robotics into Surgeries and Diagnoses
Emergent technologies are increasingly making a place for themselves in healthcare provision. Already, AI-capable software is being used to analyze large amounts of data for trends and insights. It can also be used to detect subtle nuances in test results and scans that are indiscernible to the human eye to help diagnose health conditions.
Robotic technology is being utilized in surgeries that require more precision or smaller movements than a human surgeon can perform. These technologies are rapidly expanding and iterating. Though many are still in the early stages of development and adoption, their use will continue to increase because of the clear benefits they present.
Tech Trends Continue for Patient Health and Well-Being
These technological trends and more will continue to develop and will be increasingly implemented to improve patient health and well-being in the coming years. Other technologies that are currently in embryonic or experimental stages will continue to emerge as well that will continue to shift the way tech is applied to healthcare.
It’s important to stay on top of technological solutions that are available now, as well as keep an eye on the technological horizons for significant developments that are sure to come.