Patient Identifying Information Used Determines Patient Safety Within Hospitals

Even before the COVID-19 pandemic hit the US, its healthcare system was plagued by a multitude of issues. Increasing costs, the lack of price transparency, medical identity theft, healthcare data breaches, duplicate medical records, and the lack of interoperability are just some of the many problems surrounding healthcare. While these are persistent issues, many of them took a backseat when COVID-19 struck the US – except for patient misidentification. During the pandemic, healthcare providers profoundly felt the lack of an effective patient identifier. It led to patient safety issues, result mix-ups, patient misinformation, and so on. Let’s explore what healthcare experts are doing, why a national patient identifier might not be enough on its own, and how patient identifying information used by a healthcare provider heavily influences patient safety.

The current state of patient identification
Patient identification has been a mess within the US healthcare system due to a number of factors. However, the biggest reason is that there is no standardized patient identifier that can be used to accurately identify patients’ medical records. As a result, many healthcare providers are still using the archaic process of finding electronic health records manually. Even though EHR systems provide search functionalities, issues such as common names and demographic characteristics as well as duplicate medical records make it harder to identify the accurate medical record. Thus, using names as patient identifying information is inefficient, dangerous, and, in high-stress environments such as registration desks of hospitals, might lead to misidentifications.
As a result, even this year, coalitions were formed where healthcare leaders came together to demand a state-funded UPI (Universal Patient Identifier) and expressed why accurate patient identification is crucial to ensure desirable healthcare outcomes. Back in July, healthcare leaders across the industry were relieved when the House of Representatives finally voted to overturn the ban on the UPI.
Its creation, though, depends on the Senate now; they must approve the policy change. While we are closer to a national patient identifier than we’ve been in years, the Senate didn’t approve of abolishing the ban last year, citing privacy concerns.
Why is patient identification so crucial?
Let’s take it from an expert, Tom Leary, HIMSS VP of Government Relations. During a session organized by the ONC (Office of the National Coordinator), Mr. Leary stated that incorrect patient data hampers public health response initiatives, such as those during the pandemic. As a result of patient identification errors, improper data sharing, delayed test results, and inaccuracies in medical records were seen during the crisis. Also, whenever the vaccine for COVID-19 is created, accurate patient identification is a must to deploy large-scale immunizations. While these were just some of the anomalies observed during the pandemic, patient identification errors have been rampant for years.

Hospitals using ineffective patient identifying information to identify proper medical records have been facing issues such as denied claims, patient safety issues, duplicate record creation, overlays, and poor care coordination across their facilities. With all that said, along with years of medical record errors, duplicates, and so on, will the UPI be enough on its own to eliminate all the existing issues?
Choosing the right patient identifying information won’t be enough for the UPI
Short answer: the UPI won’t be enough in the near future. First, creating a UPI will be quite expensive and time-consuming. In terms of implementation, it will take years to cover the entire population. Also, its efficacy will entirely rely on the patient identifying information used. For instance, many healthcare providers already use Social Security numbers, and they’ve proven to be ineffective identifiers. These numbers can be easily lost, stolen, or even forgotten by the patients, making them unreliable identifiers.
Thus, the only way to make the UPI a success is to couple it with an existing and robust patient identification platform, one that has experience ensuring positive patient identification. That’s where RightPatient comes in.
RightPatient uses the most practical patient identifying information
Many healthcare providers are using RightPatient as their patient identification platform, and they chose it for a number of reasons. One factor that sets RightPatient apart is it uses the one feature that cannot be stolen, forgotten, or misplaced as patient identifying information – patients’ faces.
After successfully scheduling an appointment, the patient receives an SMS or email requiring a personal photo as well as a photo of their driver’s license. RightPatient matches the photos to ensure remote patient authentication.
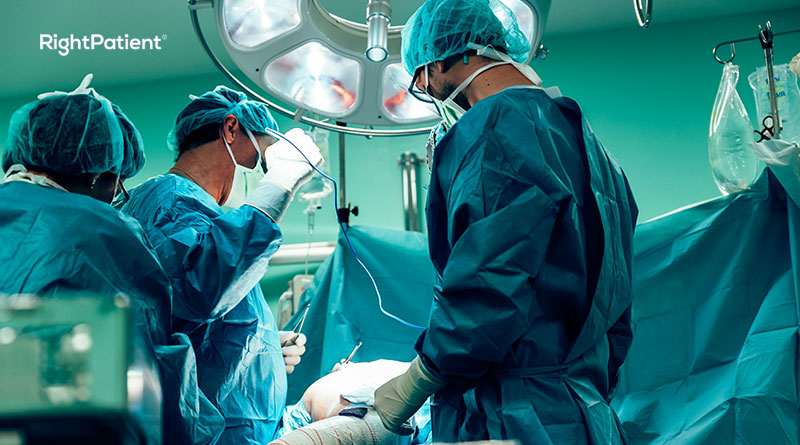
Within healthcare facilities, registered patients only need to look at the camera – the platform matches the photos and ensures accurate and touchless patient identification. This helps to provide a hygienic environment for both patients and registrars, eliminating infection control issues and enhancing patient safety.
RightPatient has years of experience ensuring accurate patient identification – try us now to learn how we can help you reduce denied claims, prevent duplicate records, improve healthcare outcomes, and more.










Leave a Reply
Want to join the discussion?Feel free to contribute!