Five Common Patient Safety Concerns Hospitals Must Address Effectively

Arguably, hospitals and health systems have been facing a very rough patch due to COVID-19, and with its latest variant, Omicron, it looks like it will continue to haunt everyone for quite some time. While COVID-19 is the biggest problem right now, it’s not the only one – healthcare providers need to address several issues to treat patients effectively and safely. With that out of the way, let’s dive deep into some of the typical patient safety concerns hospitals need to address effectively.
Five patient safety concerns hospitals need to focus on
COVID-19
Quite unsurprisingly, this tops all lists regarding patient safety concerns in the world now. This has been the most significant and unprecedented challenge healthcare providers have faced in recent years. Even with the new vaccines, rules and regulations, cases are still increasing due to the Omicron variant.
The variant has caused several hospitals to permanently close their doors, rapid changes to the entire healthcare landscape, incorporation of telehealth into the mix and adoption of other practices – desperate times call for desperate measures.
While hospitals have already allocated or built separate facilities to accommodate COVID-19 patients, surges created by new variants have overwhelmed them. During such surges, hospitals postpone non-emergency elective procedures and surgeries, limit visitors, shorten visiting hours and encourage telehealth to protect regular patients from catching COVID-19 at their facilities. While these have become the typical responses, it disrupts the healthcare experience for many patients – what if the non-emergency procedure is crucial for the patient, or what if the hospital suspends ALL elective procedures? These are some questions that need answers from healthcare providers.
Healthcare staffing issues
The virus has led to another problem – a shortage of healthcare professionals. Many professionals contracted the virus. Unfortunately, some lost their lives, and others had to isolate themselves. On the other hand, hospitals incurred huge losses since elective procedures and regular healthcare visits were postponed or canceled. They had to furlough or lay off workers and introduce pay cuts. These actions led to massive shortages as nurses and other healthcare staff members had to look after far more patients than they could manage.
This is a huge patient safety concern because fewer healthcare staff members mean that the treatment will be rushed and compromised. Patients won’t receive the level of care they need, and increased pressure on healthcare staff members might lead to mistakes.
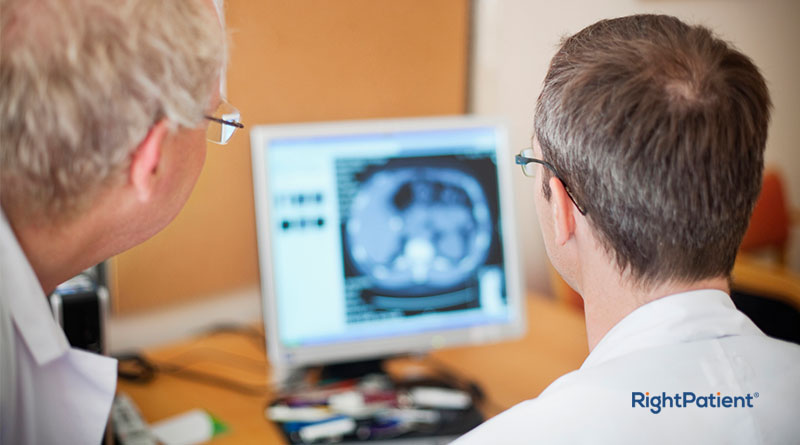
Issues with diagnoses
While diagnostic errors were common before COVID-19 wreaked havoc, the virus has caused many patients to miss out on scheduled diagnostic tests or even have them delayed. In the pre-pandemic era, errors such as delayed diagnosis, misdiagnosis and failure to diagnose related diseases were common. However, healthcare providers were forced to delay all procedures barring COVID-19 cases to allocate resources to deal with the pandemic.
Due to such delays, the patients’ health problems worsened, leading to more complex treatment plans, higher risks and chances of patient safety incidents. Once again, healthcare providers are using telehealth to address this issue. Although diagnostic tests are virtually impossible, patients need to physically come to healthcare facilities for the tests.
HAIs – one of the most significant patient safety concerns now
Hospital-Acquired Infections (HAIs) are quite problematic and have become one of the prominent patient safety concerns in the US, especially after COVID-19. Hospitals consist of patients suffering from different diseases, some of which are contagious. When other people, be it patients or healthcare staff members, have contact without ample protection, they’ll contract the virus as well. This is how COVID-19 has spread, and healthcare providers need to use innovative solutions and strategies to prevent HAIs. For instance, touchless patient identification platforms like RightPatient can help with infection control and reduce HAIs effectively – more on that later.
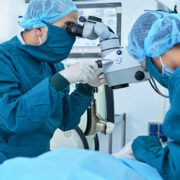
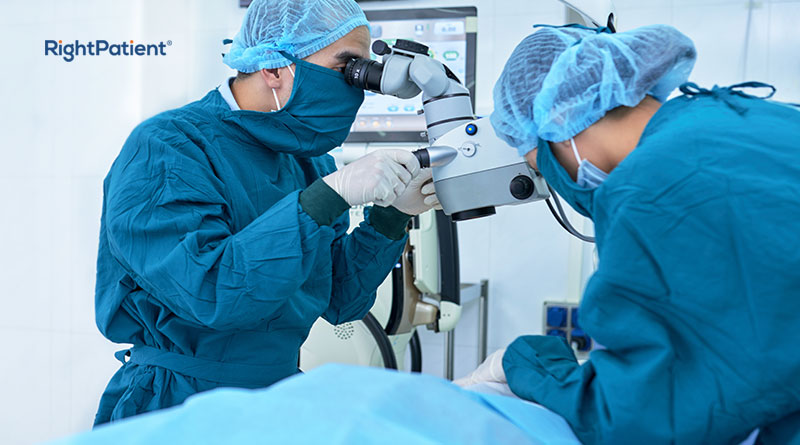
Errors during surgeries
Surgical mistakes are one of the biggest challenges for most healthcare providers. Surgical errors come in various forms, from retained surgical instruments and wrong-site surgery to operating on the wrong patient. A frequent surgical mistake is when patients get mixed up due to common names. While there are miraculous cases where the initial patient survived, these are dangerous nonetheless.
Surgical mistakes due to patient misidentification can be prevented with a tried and tested biometric patient identification like RightPatient. Using their photos, it ensures that patients are identified accurately and safely across the care continuum.
RightPatient prevents duplicate medical records and mix-ups – preventing patient safety incidents in the process.
How are you addressing patient safety concerns at your healthcare facility?