Hospital Acquired Infections are the Topmost Patient Safety Concerns – 4 Ways to Address Them

We started feeling the effects of the pandemic towards the end of 2019. The committed efforts in the US to create vaccines that would aid the hospitals and health systems in their fight against the pandemic have aided their return to a degree of normalcy. Caregivers are often concerned about the dangers of hospital-acquired infections (HAIs) as one of the foremost patient safety concerns. The cases of COVID-19 made it an even bigger cause for worry for everyone. Patients are conscious of getting infected in the hospital with the virus and with the rate at which it spreads, caregivers have to be extra committed to infection prevention. Understanding this, we can move further to look at how HAIs can be prevented in the hospital and how patients can be assessed without touching them, for instance, by using a touchless patient identity verification platform.
Addressing one of the trending patient safety concerns – HAIs
Hospitals are often perceived as a haven where people can be cared for as per their healthcare needs. However, the need to consider establishing policies to address the problems associated with patient safety concerns to forestall adverse health outcomes. Here are some ways in which hospitals can deal with HAIs.
Clean surfaces and patient equipment regularly
This is so important and almost traditional. It is one sure practice that either eradicates HAIs or reduces them to the barest minimum. Thorough cleaning and care for all surfaces in special parts of the hospitals such as where samples of blood, bodily fluids, or instruments that would be used to treat a patient are stored. Such care has to be administered to areas where people such as medics, suppliers, patients, or visitors are attended to. This will help to control the spread of germs that might have attached to their persons from outside. This is how control over infections can be achieved in the hospital.
The responsibility falls on healthcare providers to continue to institute practices that improve infection control in all facilities. Ensuring a clean environment with clean surfaces such as walls, chairs, tables, beds, doorknobs being cleaned and disinfected regularly and thoroughly. This has become even more important to do now more than ever. Disinfection of patient materials such as sheets and gowns must be carried out after each use. The use of disposable plates, cups, and spoons alone should be encouraged.
Enforce hygiene practices on everyone
One of the things we have picked from the pandemic is the consistent use of nose masks as well a practicing social distancing. That applies even in less clinical circumstances. It shows you just how crucial those practices should be encouraged within hospitals. The consequences are much dire in the case of poor hygiene practices in the hospital and health system. Caregivers will have a nightmare experience if a Covid-19 patient comes in contact with hundreds of other patients in an unprotected manner. People tend to not enjoy the use of masks, because of this set of people, it is important to enforce social distancing protocols in hospitals.
The use of signs warning against such unhygienic practices should be encouraged. A sign that reads “NO MASKS, NO SERVICE” can be placed in strategic positions in the hospital to restrict such carefree attitudes in the hospital. Informative designed posters can be used to educate people on the social distancing protocols should also be used. Hand sanitizers should be made available and compulsory for anyone who wants to enter the clinic. Maintenance might be costly but it is worth the effort nonetheless.
Workers in the hospital must project adherence to these rules for patients to emulate by maintaining hand hygiene, use masks, and maintain social distancing. New workers must be adequately trained and enlightened about the essence of a clean and disinfected environment.
Have a robust and updated infection control policy in place
The above-mentioned practices are but a few that help to maintain infection control protocols being administered by a standard caregiver. These policies must be renewed and retaught regularly enough and they must be shared with staff members to prevent HAIs.
Other recognizable practices that are commonly an important infection control policy include
- The use of gloves
- Use of personal protective equipment
- Regular and proper disposal of weight
- Ensuring proper etiquette while coughing
- Avoiding needlestick sores and injuries
Using contactless solutions to prevent prominent patient safety concerns
Providing quality care and ensuring patient safety as a practice is extremely difficult and important. In improving patient safety and quality of care, multiple solutions can help care providers reduce HAIs and deal with other patient safety concerns such as poor identification of patients or a case of mistaken identity.
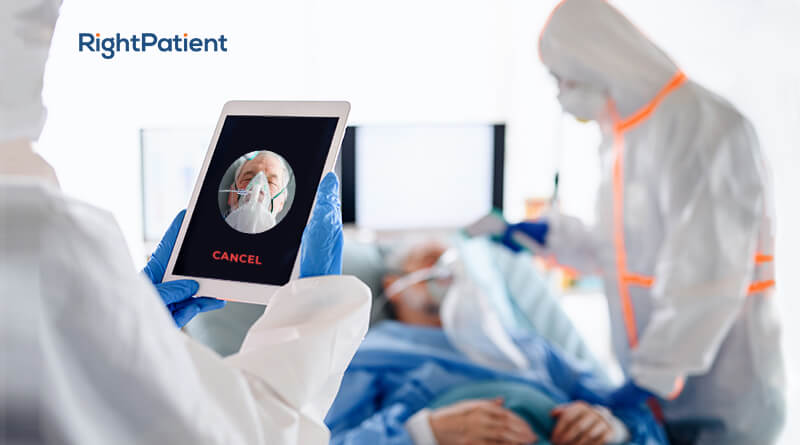
One of such solutions available is RightPatient, a touchless biometric patient identification platform that helps identify patients in any care situation and time. It also does this in a simple, safer, and more hygienic manner. The patient only needs to gaze at the camera to register and on subsequent visits by the care provider staff. The platform compares the live photo with the saved one and displays their accurate medical record after the match is found.
It significantly minimizes the dangers of infection control issues, prevents medical errors, reduces misidentification of patients and other patient safety concerns. It played an active role in the post-pandemic scenarios but it has been in existence for years in some health institutions because it has no deleterious effects attached to its usage.
Question is, what are you using to accurately identify patients and reduce HAIs in the healthcare systems while doing it?



















 RightPatient is the healthcare industry’s leading photo-based biometric
RightPatient is the healthcare industry’s leading photo-based biometric