Understanding Abnormal EKG Findings Without Jumping to Conclusions
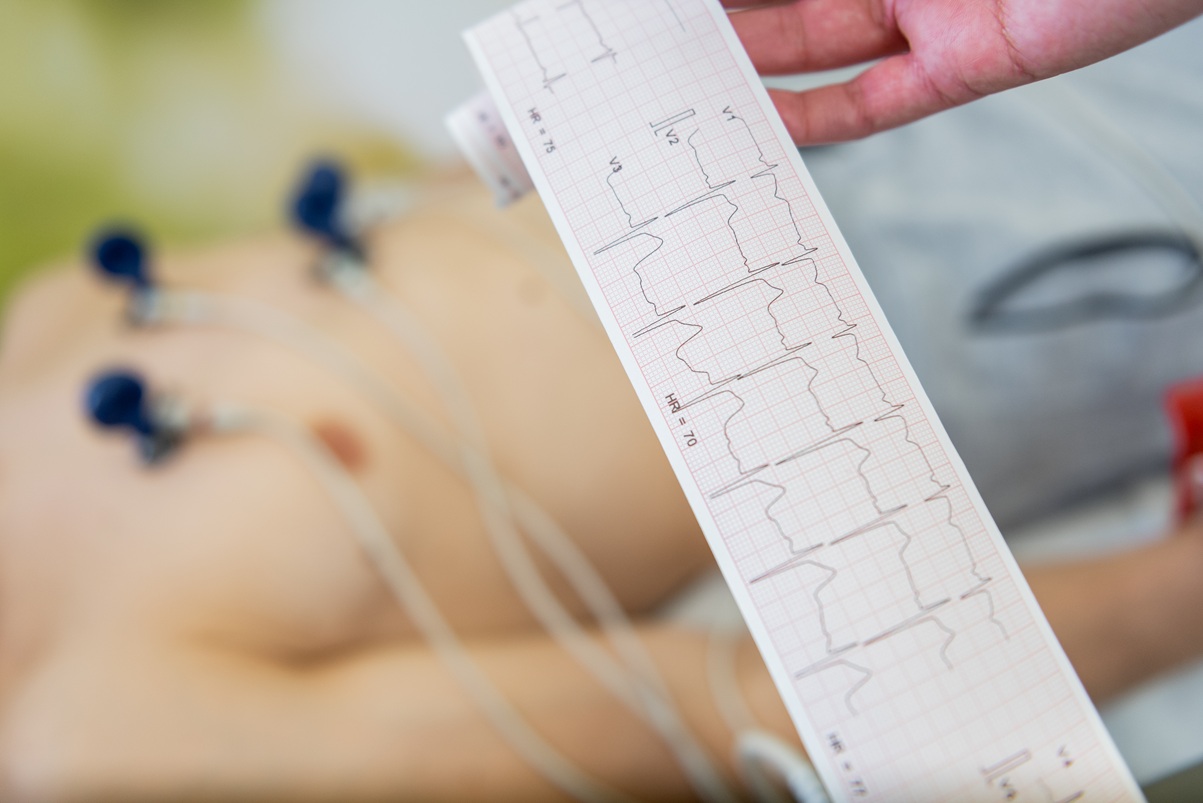
If you’ve ever had an EKG done and the doctor told you that your EKG is abnormal, then I’m sure you know how it feels. Most people tend to jump to the worst possible conclusion about an abnormal EKG. It doesn’t help that most people don’t know much about what an EKG is or how to interpret the results.
Fortunately, there are many reasons why an individual might experience an abnormal EKG, and not all of them represent life threatening conditions. In this article we’ll explore what can cause abnormal EKG readings, what an EKG can and can’t tell you, and how you can distinguish between what requires an urgent visit to the doctor and what can be dealt with in a calm and relaxed manner.
What an EKG Really Tells Us About the Heart (and Why “Abnormal” Is So Vague)
An EKG is essentially a snapshot of the heart’s electrical activity using small electrodes placed on the surface of the skin. What’s important to understand is that an EKG is essentially one picture in time. When a doctor says that “the EKG is abnormal”, he/she could be referring to a number of things, including:
- Irregular heart rhythms (either too fast or too slow)
- Irregular heart rhythms or where the heartbeat begins
- How quickly the electrical impulse travels through the heart
- Waveforms that indicate some level of heart strain, reduced blood flow to the heart, or injury to the heart muscle in the past – although these can be non-specific
At times, the abnormal part may be trivial, temporary or have nothing to do with the heart. As a result, many clinicians will obtain another EKG, compare the current EKG to previous ones, or schedule a monitoring session.
Normal Variables That Can Cause an EKG To Show Differences While the Heart is Normal
Those looking for answers on what causes an abnormal EKG are usually surprised at the number of normal, everyday variables that can make a difference in the EKG results. Some examples of these variables include:
- Lead placement and physical characteristics of the body. If EKG leads are placed slightly differently, or the shape and size of the body, chest wall, or skin contact differs, it can affect the results of the EKG reading. Similarly, movement, shaking, or tension while taking the test can also affect the results of the EKG.
- A Transient Increase in Heart Rate. Stress, pain, fever, dehydration, caffeine, nicotine, or inadequate sleep can elevate your heart rate. Rapid heart rates can alter waveform shapes, especially if you were anxious during the test.
- Breathing Patterns. Taking deep, rapid breaths, or holding one’s breath, can temporarily affect heart rate and rhythm. Some people feel short of breath solely because of their own worry – and this can affect the tracing.
- “Normal Variants”. Some EKG patterns are simply normal for some people – for example, if you are young, physically active, or have a naturally slower resting heart rate.
None of these are invalid of the need for follow-up. However, they do explain why an “abnormal” result does not mean a diagnosis has been made.
Next Step: If you were stressed, caffeinated, ill, or sleep-deprived while taking the test – write that down – it’s relevant background information.
Common Medical Factors That Contribute to Heart Problems
There are many different medical factors that contribute to an abnormal EKG. Some of these are relatively rare and serious; some are more common and treatable.
- Arrhythmias (Changes in Rhythm). An EKG can detect irregular patterns of rhythm, including atrial fibrillation, ectopic beats, or a rapid heart rate beginning in the upper chambers of the heart. Some arrhythmias occur intermittently, and therefore a normal EKG does not rule out their presence. On the other hand, an abnormal EKG may necessitate long-term monitoring of the rhythm.
- Variability in Electrical Pathways. Occasionally, the electrical “cables” of the heart will transmit impulses more slowly (or via an alternate route). This may show up as an abnormally wide waveform, or as an abnormally short cable signature – and, based on the degree of your symptoms, this may require consultation with a cardiologist.
- Prolongation of the QT Interval. The QT interval reflects the time required for the heart’s electrical recovery and resetting between beats. An abnormally prolonged QT increases the probability of developing dangerous rhythms under specific conditions – especially when combined with use of specific medications, low levels of certain electrolytes, or an existing susceptibility to arrhythmias.
- Evidence of Reduced Blood Flow or Increased Load on the Heart Muscle. Certain waveforms can suggest reduced blood flow to the heart muscle, or excessive workload on the heart muscle. These waveforms require clinical correlation – patient symptoms, patient risk factors, and possibly additional testing.
It is understandable if this appears to be a great deal to comprehend. You do not need to turn this into a personal research project. Your task is to note any unusual symptoms and develop questions – your clinician’s job is to connect the dots between the various pieces of data.
Next Step: Ask whether the finding is “new”, “mild”, or “requires emergency attention”, and what rationale was applied to support that determination.
Medications, Supplements & Substances That Can Change Your EKG Results
Another key factor that helps to answer the question of what causes an abnormal EKG is what is currently in your system – prescription medications, over-the-counter medications/supplements, and substances that influence your heart rate or timing of electrical impulses.
Some prescribed medications may prolong the QT interval, or create conditions that may lead to dangerous arrhythmias in high-risk patients. This does not mean that a medication is “bad”, or that you must discontinue its use immediately. Rather, your clinician may:
- Assess your full medication regimen (including as-needed medications)
- Obtain laboratory tests (such as electrolyte measurement – e.g. potassium and magnesium) to investigate possible concerns
- Obtain a repeat EKG or monitor your rhythm if you are symptomatic
Other substances, such as stimulants (for instance, caffeine consumed excessively), nicotine, decongestants, and some energy-based products can also increase heart rate and induce palpitations that can be seen in the tracing.
Next Step: Compile a complete listing of all prescription medications and supplements (with photos of packaging) to carry to your appointment – the specifics matter.
Why People Get Panicked and How It Affects Their EKG
In addition to the more obvious health-related explanations of what causes an abnormal ekg, for many adults, the explanation is simply this: they got freaked out, felt chest tightness, experienced palpitations and then went in to have the test, and now the test results are feeding their fears.
Anxiety and panic can activate your body’s fight or flight response. Anxiety and panic can cause:
- Increased Heart Rate
- More Obvious and Forceful Beats
- Tightness in the Chest from Muscular Tension
- Light headedness due to changes in breathing
While these symptoms are real, and can be frightening, they are also similar to the symptoms that clinicians commonly associate with cardiovascular disease – hence, getting an evaluation is the best way to address the symptoms.
To ensure that the primary reason for your anxiety is not your imagination, the next step is to ensure that your symptoms were not caused solely by your anxiety.
If you want an educational, calming explanation of how anxiety and heart-related symptoms can be associated – and why an EKG may look abnormal during episodes of extreme stress – this overview of what causes an abnormal EKG will give you a better platform for discussing your symptoms in a calmer fashion with your medical team.
Next Step: If your symptoms are triggered by stress, try documenting “stress trigger + symptom + duration” for a week – it will give your clinician something concrete to work with.
When an Abnormal EKG Requires Emergency Treatment
Most abnormal EKG findings are not emergencies. However, there are times when an abnormal EKG warrants immediate treatment. Obtain emergency treatment (your local ER or emergency number) if you have an abnormal EKG and any of the following:
- Chest Pain or Pressure That Doesn’t Go Away Immediately, Especially Accompanied by Sweating, Nausea, or Shortness of Breath
- Blackouts or Close Calls with Losing Consciousness
- Severe New Shortness of Breath, Even at Rest
- Confusion, Significant Weakness, or Symptoms Which Are Clearly Getting Worse
- Unusual or Fast Heart Beat Which Won’t Slow Down, Especially With Dizziness or Chest Discomfort
If you’re unsure, it’s perfectly reasonable to err on the side of caution and seek emergency medical treatment when symptoms seem severe.
Next Step: Add a simple reference to your cell phone: “Abnormal EKG + Loss of Consciousness/Chest Pain/Shortness of Breath = Immediate Medical Attention.”
What Your Doctor Will Probably Do Next (and What to Ask)
Because what causes an abnormal EKG can range from harmless to serious, most subsequent steps are designed to narrow down the possibilities – without instilling panic.
Several subsequent actions your doctor may consider:
- Multiple Repeat EKGs (particularly if the initial lead placement and/or stress may have affected the results)
- Monitoring of the Rhythm Over Time (Holter monitor or event monitor)
- Laboratory Testing (assessing electrolyte levels, thyroid hormone levels, etc.) to investigate your symptoms
- Echocardiography (ultrasound examination of the heart) to evaluate the structure and function of the heart
- Review of Medications and Risk Assessment (if QT interval changes are noted).
Questions you may wish to ask:
- “What exactly was abnormal — rate, rhythm, QT, or something else?”
- “Is this new versus previous EKGs?”
- “Do these findings correlate with your symptoms — or could they be coincident?”
- “What would prompt an urgent intervention — and what would wait until the time you see us in clinic?”
You do not need to ask all of these questions at once. Asking a single thoughtful question can go a long way to reducing uncertainty.
Next Step: Write the two most important questions you’d like to ask your physician on a piece of paper before your next appointment — so that anxiety does not erase them during the meeting.
Conclusion
An abnormal EKG is a signal to pay attention—not a verdict. In many cases, what causes an abnormal EKG turns out to be temporary factors, normal variation, anxiety-related changes, medication effects, or rhythm patterns that can be evaluated step by step. If your mind keeps trying to sprint ahead, it can help to bring it back to the practical: What did the report actually say, what symptoms do you have, and what does your clinician recommend next?
Safety disclaimer:
If you or someone you love is in crisis, call 911 or go to the nearest emergency room. You can also call or text 988, or chat via 988lifeline.org to reach the Suicide & Crisis Lifeline. Support is free, confidential, and available 24/7.







Leave a Reply
Want to join the discussion?Feel free to contribute!