Understanding the Growing Demand for Professionals in Psychological Care

Mental health is everywhere in conversation today—celebrities share their struggles, coworkers talk about stress, and news reports highlight rising depression rates. Society now recognizes mental well-being as essential, yet there aren’t enough professionals to meet the growing demand for care. Long wait times, provider shortages, and increasing workplace stress have made access to psychological support a serious challenge. As mental health care evolves with new policies and training advancements, the need for qualified professionals has never been greater.
In this blog, we will explore what’s driving this demand, how the field is changing, and why the next generation of experts will play a central role in its future.
The Mental Health Crisis Is Reshaping the Workforce
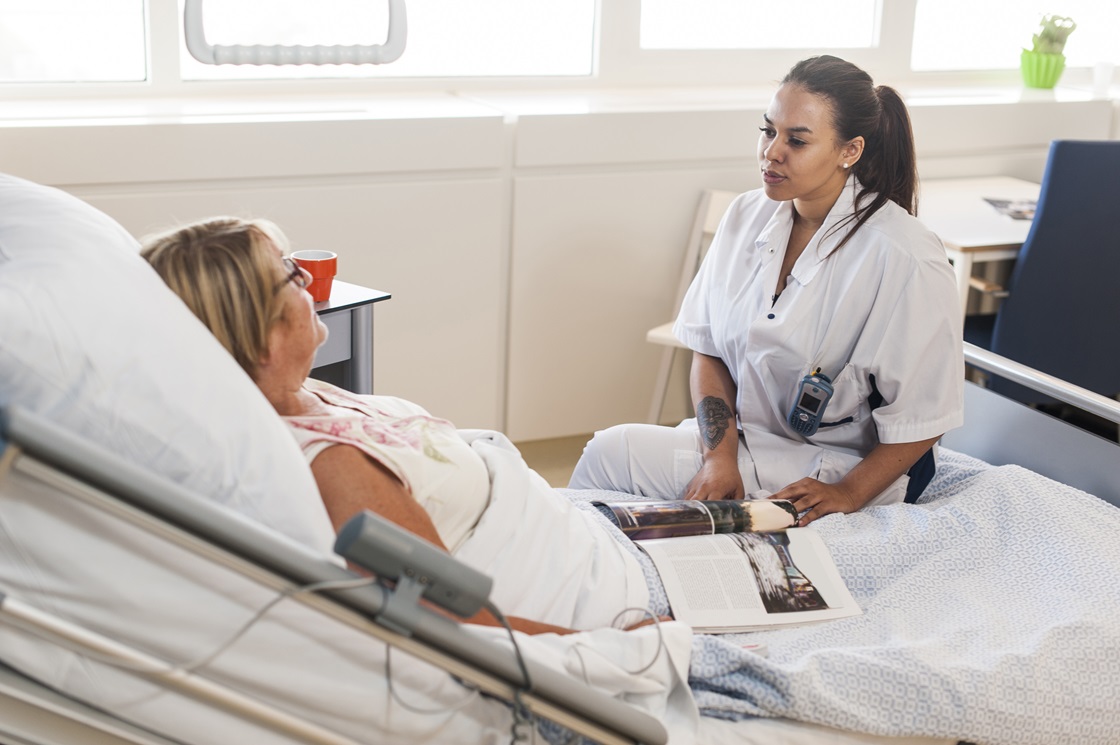
Mental health is no longer an afterthought—conversations about anxiety, depression, and stress are everywhere. The stigma around seeking help has faded, but the demand for care has outpaced the number of available professionals. Many people face long wait times for therapy, and in rural areas, access to mental health providers is even more limited.
Workplace stress has also fueled this crisis. Companies now see mental health support as a necessity, but without enough professionals, these programs can’t serve everyone in need. The same is true for schools, where rising anxiety and depression among students have created a demand for more counselors and psychologists. Despite growing awareness, the shortage of trained experts remains a major barrier to care.
The Growing Need for Highly Trained Psychologists
The demand for mental health professionals isn’t just about filling positions—it’s about ensuring quality care. As the field expands, there is a greater need for highly trained psychologists who can provide evidence-based treatments and specialized care.
This is where APA-accredited PsyD programs play an instrumental role. These programs make sure that students receive the highest level of education and clinical training, preparing them to handle complex psychological issues. As mental health challenges become more nuanced, professionals must be equipped with the right skills, ethical understanding, and research-based approaches to provide effective care. Plus, the accreditation by the American Psychological Association (APA) ensures that the degree meets the highest educational and ethical standards.
Psychologists today do far more than just traditional therapy. They work in hospitals, schools, corporate offices, and even the legal system. Some focus on trauma care, helping individuals recover from life-altering experiences. Others specialize in behavioral psychology, aiding those with developmental disorders. The modern mental health landscape requires experts with in-depth knowledge across various fields, and quality training programs are essential to meeting this need.
Governments and healthcare organizations are beginning to recognize this reality. Efforts to expand mental health training programs, offer financial incentives for students entering the field, and increase funding for psychological research are gaining traction. However, these efforts must continue to grow to match the rapidly increasing demand for care.
Why the Shortage of Professionals Affects Everyone
It’s easy to think of the mental health crisis as someone else’s problem. But in reality, the shortage of trained professionals impacts everyone. When people can’t get the help they need, the effects ripple across society.
For businesses, unaddressed mental health issues lead to lower productivity, higher absenteeism, and increased healthcare costs. Employees who struggle with anxiety or depression without proper support are less engaged and more likely to leave their jobs. This results in high turnover rates and added strain on the remaining staff.
In healthcare settings, the lack of psychologists puts additional pressure on doctors and nurses, who are already overwhelmed. Many physical health issues have psychological components, from chronic pain to recovery after surgery. Without mental health professionals available, medical providers must fill the gap, often without the necessary training.
The justice system also feels the strain. Courts increasingly recognize the importance of psychological evaluations in legal cases, but there aren’t enough forensic psychologists to handle the caseload. In prisons and juvenile detention centers, a lack of mental health professionals means many individuals don’t receive the care they need, leading to higher recidivism rates.
Even at the community level, the shortage is apparent. Schools with too few counselors see higher rates of behavioral issues and declining academic performance. Families struggling with mental health challenges often don’t have access to support, leading to increased stress and instability at home.
The Future of Psychological Care
The mental health field is evolving rapidly, and the professionals entering it now will shape the future of care. New technologies, like teletherapy and AI-driven diagnostic tools, are helping to bridge the gap, making services more accessible. However, technology alone won’t solve the problem—there is no substitute for well-trained human professionals.
Addressing the shortage requires a multi-faceted approach. Expanding training programs, increasing funding for mental health initiatives, and improving working conditions for psychologists are all critical steps. Encouraging more students to pursue careers in psychology by offering scholarships and loan forgiveness programs can also help attract talent to the field.
Public policy must also shift to prioritize mental health. Governments need to ensure that funding for mental health services keeps pace with demand, particularly in underserved communities. Insurance companies must make mental health care more accessible and affordable. Schools, workplaces, and healthcare systems all need to integrate mental health support into their structures more effectively.
Most importantly, the cultural shift toward recognizing the importance of mental health must continue. The more people understand the value of psychological care, the more pressure there will be on institutions to make it accessible. The conversation has started, but real change will require continued advocacy and investment.
The bottom line? The demand for mental health professionals isn’t just growing—it’s reaching a critical point. As society becomes more aware of the importance of psychological care, the need for trained experts will only increase. Without enough professionals in the field, millions will continue to struggle without adequate support.
The good news is that solutions exist. Expanding access to quality education and training, improving workplace conditions for mental health providers, and increasing public investment in mental health services can all make a difference. The future of psychological care depends on the professionals who step up to meet this challenge.
If the past few years have shown us anything, it’s that mental health can’t be ignored. The time to invest in psychological care isn’t tomorrow—it’s right now.