Top 5 Questions For Biometric Patient ID Vendors

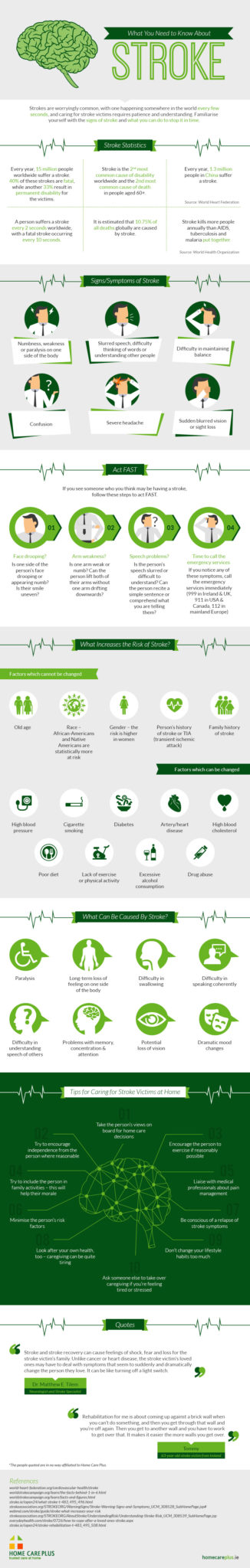
Biometric patient ID solution deployments to increase patient safety, eliminate duplicate medical records, and prevent medical ID theft and healthcare fraud are spreading rapidly throughout the healthcare industry. More medical facilities are researching the implementation of biometric patient ID in response to the increased attention and negative downstream impact caused by misidentification and the push to achieve 100% patient ID accuracy in healthcare.

Learn the top 5 questions to ask when researching biometric patient identification solutions.
While the front end benefits of implementing biometrics for patient identification may be clear, what often may be slightly fuzzy is the back end technology of biometric patient ID systems and just what exactly the technology is actually capable of achieving. Biometric technology is not static, and depending on which modality a medical facility chooses, the ability to achieve some of the aforementioned benefits may be limited.
As a biometric vendor with over 14 years of experience in biometrics, cloud-computing, integration, and large-scale project implementations, we understand the technology and its capabilities and limitations. We know what certain biometric modalities are capable of, and are well positioned to offer educated recommendations on the best and most effective biometric technology for patient identification in healthcare. Unfortunately, many misunderstandings of biometrics exist that could influence decisions to adopt the technology to improve patient safety in healthcare.
Never fear! We are here to help make sense of biometrics for patient ID in healthcare by offering advice on the top 5 questions hospitals and medical facilities should be asking during the research phase of their due diligence to implement the most effective and sustainable solution. Here are our top 5 questions you should ask when researching biometric patient ID solutions:
- Does a patient have to physically touch a biometric hardware device to be enrolled and identified?
Why this is important: Patient hand hygiene is terrible. In fact, Dr. Lona Mody and her research team at The University of Michigan recently released a study that reported: “One-quarter of patients (24.1 percent) had at least one multidrug-resistant organism (MDRO), or superbug, on their hands when they checked in.”Hospitals have a responsibility to ensure the cleanliness of any new devices introduced as part of the patient check-in or care process that require patient contact to support infection control protocols. The rise in awareness of the dangers that hospital-borne infections cause should call into question patient safety issues that contact-dependent biometric pose, especially in light of the dangers that MRSA, Ebola, and other germs and illnesses that can be spread by contact. Think about a patient who may be pregnant and not realize it who contracts an illness that jeopardizes the safety of themeselves and their child simply by touching a device that wasn’t properly cleaned?
Implementing contact-dependent biometric hardware requires medical facilities to ensure that the device is properly sanitized. Hospitals who see an average of 350,000 patients per year could be facing an extra $38,000 in sanitation expenses after implementing a contact dependent biometric hardware device.
The use of contact dependent biometrics can also have a negative impact on patient acceptance. Patients unwilling to touch a device will most likely decline to use the patient identification system. Since patient acceptance and participation is voluntary and the goal is to maximize their use of the technology to drive incremental value, this should be a concern for medical facilities.

- Is the back end biometric technology based on one-to-many or one-to-few segmented searches?
Why this is important: The only true way to prevent duplicate medical records and tangibly improve patient safety and patient data integrity through a biometric patient identification solution is to implement a system based on a one-to-many (1:N) search. Biometric patient ID systems based on a 1:N search compare a captured biometric template against ALL stored templates in the biometric database during enrollment.
Alternatively, a one-to-few segmented search (1:Few) compares a captured biometric template against a portion of the total biometric database; hence, a credential (such as date of birth) needs to be provided prior to the biometric scan to determine which templates should be compared against. The biometric system would then compare the captured template against only those templates that share the same birth date.
This is an extremely important question to ask when vetting biometric patient identification solutions. If the premise of implementing biometrics to identify patients is eliminating duplicate medical records, prevention of medical ID theft, and to improve patient safety, solutions based on a 1:Few search do not have the ability to deliver.
- Can the biometric patient ID solution recognize patients from any encounter end point?
Why this is important: In the old days, healthcare delivery seemed much simpler. You get sick or suffer an ailment and drive to the doctor’s office or hospital. Treatment is rendered. You go home (or rehab if needed). However, modern healthcare and the digitization of care delivery has radically changed the complexion of how, when, and where we receive services. We now have the ability to login into patient portals 24/7 to view, read, or download data. Telemedicine visits allow us to receive care without every leaving the comfort of our couch. mHealth apps place medical advice, care services, and protected health information (PHI) data access in the palm of our hands.
These examples represent just a few of the new touchpoints along the care continuum that have blossomed in popularity witnessed by the digitization and personalization of healthcare. Although these examples shed light on the new reality of healthcare, accurate patient identification becomes no less important prior to accessing these new touchpoints. The problem is that not all biometric patient ID solutions have the ability to address accurate patient ID at every new touchpoint. Most are built and designed to handle patient ID in one venue and one venue only – face to face patient registration in brick and mortar environments.
If achieving accurate patient ID prior to accessing sensitive PHI or administering services through a new touchpoint along the care continuum is just as important as accurate patient identification at the point of service, why would you want to invest in a solution not built on a centralized model for strong identification wherever a patient may be?
- Does the biometric patient ID solution have the ability to instantly identify unconscious patients?
Why this is important: Many hospitals and medical facilities like the idea that a biometric patient ID solution can identify unconscious or disoriented patients. It’s a big selling point and with good reason — patients who arrive unconscious or disoriented without identification or a family member present pose a serious risk. What if the patient is allergic to a medication? What if they have a pre-existing condition that could adversely affect or complicate treatment rendered?
Certain biometric patient ID solutions have the unique ability to instantly identify unconscious patients but not unless they use 1:N back end searches (see #2 in this post). When seconds can mean life or death, you may not want to invest in a biometric patient identification solution using 1:Few segmented searches because then clinicians will have to guess a date of birth age prior to scanning the patient’s biometric credentials. Back end search limitations can delay the identification of an unconscious or disoriented patient.
- What age groups are eligible to use the biometric patient identification solution?
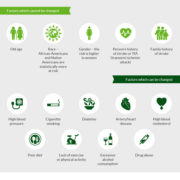
Why this is important: As mentioned earlier, a key metric to drive incremental value for any biometric patient ID solution is patient participation. Depending upon the back end biometric technology, not all patients are qualified to enroll in the system. Some biometric patient ID solutions recommend not to enroll patients under a certain age and others will require a larger investment in hardware to enroll younger patients who must then be repeatedly re-enrolled as they grow older and their biometric attributes change.
Biometric patient ID systems exist to protect patients from the dangers of misidentification which include, but are not limited to:
–duplicate medical records
–overlays
–medical identity theft
–healthcare fraudConsidering the fact that no patient is exempt from the risks that jeopardize their safety when not identified accurately, the post implementation goal should be to maximize patient enrollment, regardless of what age they may be.
Did you know that children as young as pre-conception are in danger of being medical identity theft victims? Biometric patient identification systems that restrict enrollment based on age are not valuable. This is an important question to ask.
Investing in a biometric patient ID solution is an exercise in educating yourself about what these systems can and cannot accomplish. While no system is perfect or a panacea to solve all the problems of patient misidentification, achieving higher quality healthcare and improving patient safety are attainable goals that can be reached when the right solution is deployed. Be cautious when researching and make sure you are asking these 5 questions!